At Mitchell’s, we care about the health of all our community family. Schedule your review today at our friendly pharmacy.
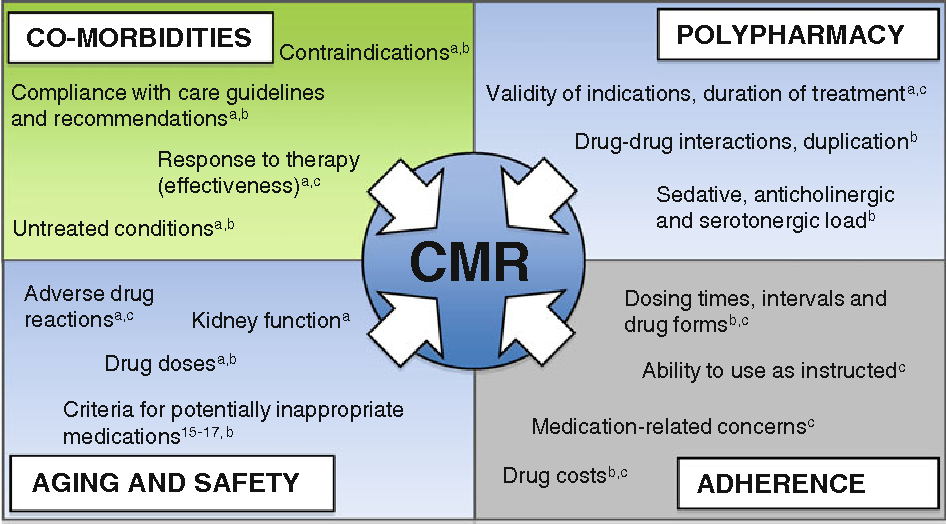
A comprehensive medication review (CMR) is an encounter conducted face-to-face or via telephone between a patient and their pharmacist. The pharmacist collects patient-specific information to identify medication-related issues and creates a plan to resolve them, alongside the patient and/or prescriber.
CMRs allows the patient and pharmacist to work together to improve patients’ knowledge of their medications, empowering patients to take ownership of their health. CMRs, unlike targeted interventions that address one condition or a single medication, are all-inclusive and can be time-consuming. A thoroughly executed CMR can take as long as 45 minutes to 1 hour.
All medications and relevant medical conditions are evaluated. Action plans are developed, and patients are periodically reassessed. You should receive a CMR at least once a year. If your medications change frequently or you have been admitted to the hospital several times recently, you may benefit from more frequent CMRs. CMRs are a free service offered by your pharmacy. Ask your pharmacist about scheduling a CMR today!
What are the benefits of a comprehensive medication review?
Each patient is unique, with a different set of health concerns, a list of medications, allergies, social barriers, and needs to be met. Medication reviews allow your pharmacist or another healthcare provider to specifically address your “differences” and optimize your care. In 2019, an online article discussed the following 8 benefits of comprehensive medication management3:
● Medication Assessment – Patients’ medications, both prescription and over-the-counter, are evaluated to determine if appropriate and effective at treating medical conditions and achieving goals of care.
● Personalized Therapy — Care is customized to meet the needs of each individual patient.
● Collaborative Care — Healthcare professionals, including pharmacists, providers, and nurses work together to offer optimal patient care.
● Patient Engagement — Involving patients in discussions and decisions regarding their medical care allows them to take ownership of their health, promoting improved outcomes.
● Ongoing Regimen Review — Patients are periodically reassessed for changes in medication regimens, control of symptoms, and progress toward goals. This creates an environment for longitudinal care or care over a period of time.
● Improved Outcomes — Improved medication adherence and greater control of chronic diseases, reduces hospital admissions/ED visits, and enhances patients’ quality of life.
● Reduced Costs — Patients only pay for medications that are necessary for their health. Improved medication adherence and decreased adverse events reduce hospital admissions, ED visits, and overall healthcare expenses.
● Increased Satisfaction — Patients receive better care for a fraction of the price, while providers witness better outcomes for their patients.
Am I eligible for a comprehensive medication review?
In 2015, a study funded in part by the National Institute on Aging looked at the increased prescribing of medications in the older adult population. Nearly 40% of these patients were on at least 5 medications.4 The most common medications noted were statins for high cholesterol, anti-hypertensive agents, diabetic medications, and antidepressants. Polypharmacy or the use of several medications at once has been shown to increase medication nonadherence and increase the risk of drug duplication, drug-drug interactions, and adverse drug reactions. Patients on numerous medications, regardless of age, are prime candidates for medication reviews. Your pharmacist can help determine if you are taking any unnecessary drugs if your symptoms are controlled on your current regimen, and ensure that each medication is being used properly.
“Transitions of care” has become a hot topic in healthcare in recent years and refers to the movement of patients between multiple providers and settings as their conditions and healthcare needs evolve.5 For example, a patient discharged from the hospital into a rehab facility, then eventually back home following a stroke. These transitions are typically complicated by poor communication between care providers, lack of patient education, and failed collaborative care. Medication reviews in these patients allow the pharmacist to help bridge gaps in care. Your pharmacist can take the time to sit down with you and explain the changes that have been made in your medication regimen. They can develop strategies to help you take your medications as directed and clear up any uncertainties.
Medication reviews are a free service offered by your pharmacy. Although the patients mentioned above may benefit the greatest, anyone who would like a medication review is eligible.
Who will be completing my comprehensive medication review?
Pharmacists pride themselves on being the “medication experts” and are excellent sources of information for both prescription and over-the-counter medications. Their education is focused on assessing medication-use for appropriateness, effectiveness, and safety to help prevent and resolve medication-related problems.6 This training, along with the idea that over 90% of Americans live within 5 miles of a community pharmacy,7 make them an obvious player in medication reviews. Your pharmacist may conduct the review, but a successful review does not stop there. A medication review is an umbrella term, which includes interventions carried out by various healthcare professionals such as providers, pharmacists, nurses and/or medical assistants.8 It is a team effort to ensure each patient receives the best care possible. A nurse may collect a list of your medications during an office visit or at hospital admission to provide to the pharmacy. They may review your discharge summary and notate changes in your regimen. A provider may prompt conversations and conduct examinations to determine which medications should be added, adjusted, or removed based on your current health needs. A pharmacist may review prescriptions prior to dispensing them, assessing for correct dosage and indication, and providing patient counseling when warranted. This integrated approach allows the puzzle pieces to come together so that optimal patient care is provided.
How to prepare for a comprehensive medication review.
You have been scheduled for a medication review with your pharmacist, either in-person or via telephone… now what? Preparing for a medication review, as a patient, is simple. Collect and bring all of your medications, both prescription and over-the-counter, and any devices, such as inhalers or insulin pens with you.9 It is important to include all vitamins and herbal supplements, as some of these cause significant drug-drug interactions. “Over-the-counter” does not always mean “safe.” Prior to the review, think about how you take each medication. Are they effective or do they make you feel worse? Have you noticed any side effects? If you regularly monitor your blood sugar or blood pressure, what are your recent readings? Are you having difficulty remembering to take your medications? Write all of this down, as well as any questions you may have and prepare to be honest with yourself and your pharmacist.
Your pharmacist has likely prepared for the medication review, as well. They may have already gathered a comprehensive medication list from your providers, confirmed disease states, evaluated fill history, and identified potential medication-related issues.10 This allows the pharmacist to establish a game plan and prioritize the objectives of the review to create an effective and efficient encounter.
What to expect following a comprehensive medication review.
Follow-up is a key component of a medication review. Your pharmacist may elect to follow-up within a few days or months, depending on the severity of issues identified during the review. Follow-up allows the pharmacist to monitor progress towards goals, ensure resolution of issues, and identify any new medication-related problems.
Many pharmacists will create a handout or takeaway for you at the conclusion of your encounter, including an up-to-date medication list and medication action plan (MAP). The MAP provides an overview of what was discussed and guidance on how to achieve patient-centered goals, including non-pharmacological options or lifestyle changes.
At Mitchell’s Drug Stores we feel we are family and we are committed to ensuring we have a happy and healthy family.
At Mitchell’s Drug Stores we feel we are all family and we are committed to ensuring we have a happy and healthy family.